Part 1: Introduction
1.1
In this Part, we discuss:
- the purpose of our audit;
- what we audited;
- what we did not audit;
- how we carried out our audit; and
- the structure of this report.
The purpose of our audit
1.2
Mental health problems affect New Zealanders from all walks of life, with one in five people affected each year. The number of people accessing specialist mental health services has been increasing steadily since at least 2003.
1.3
We carried out a performance audit that focused on the relatively few people who are most unwell with mental health problems and require a high level of care, including care in a hospital-based inpatient unit. We looked at whether:
- planning for these people's discharge from an inpatient unit to community care was completed as intended;
- the needs identified by discharge planning were followed up after discharge; and
- discharge planning was helping to improve outcomes for people with acute mental health problems.
1.4
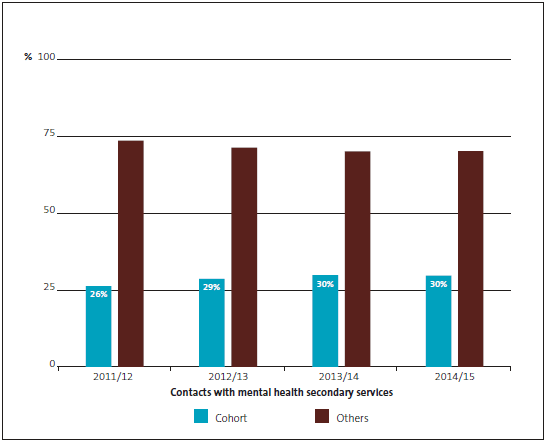
Figure 1 shows the proportion of the total population that experience mental health problems and that access services at different levels. Most people receive mental health care services in primary health care settings, usually with their general practitioner (GP). However, more than 160,000 New Zealanders (3.5% of the population) accessed specialist mental health and addiction services in 2015. About 15,000 (9%) of these people were admitted to an inpatient unit. These 15,000 people required a high level of care. When they were admitted, many were considered to pose a serious danger to themselves or others as a result of their mental illness. Some of them were admitted under a compulsory treatment order.
1.5
Providing inpatient care is expensive. District health boards (DHBs) spend a significant amount of their specialist mental health funding on inpatient units. Sometimes DHBs offer alternatives to inpatient treatment that support people to stay in the community. These can help to reduce the pressure on inpatient units.
1.6
It is important that people receive good planning and appropriate follow-up for their discharge from hospital care and transition back to the community. International evidence shows that good planning for the transition from inpatient units to the community is critical in effectively supporting people with mental health problems.
Figure 1
Proportion of New Zealanders who experience mental health problems and access specialist mental health services
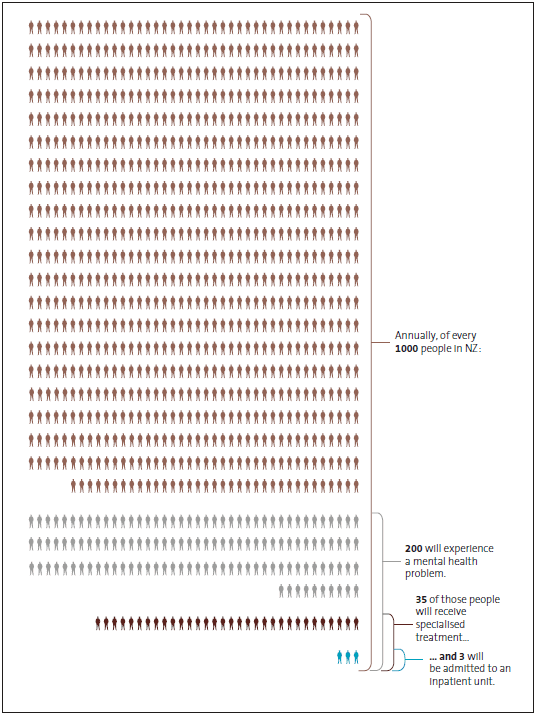
Source: Our analysis of available data.
1.7
People who need to stay in an inpatient unit often have a broad range of other needs. These can include help with accommodation or finances, or support for their employer or family.
1.8
Once a person's needs are identified, prompt access to suitable support is critical. Without this, any benefits gained from treatment during an inpatient stay are more likely to be lost, and there is a risk that the person might suffer a relapse while waiting for help to meet their other needs.
What we audited
1.9
Our audit looked at whether:
- discharge planning for people who were leaving an inpatient unit was done in a way that made sure all their relevant needs were identified; and
- people received support to make sure their mental health and broader needs were met after they left an inpatient unit.
What we did not audit
1.10
We did not audit:
- the delivery of primary mental health services;
- the experiences of people who accessed only specialist community mental health services;
- services for children and young people or adults aged 65 years or older;
- forensic mental health services;
- the experiences of people who accessed only addiction services; or
- equity of service delivery across ethnic groups or culturally appropriate services.
How we carried out our audit
1.11
Some parts of our audit looked at national information from all 20 DHBs. We also selected three DHBs to visit and audit in more depth. These visits took place between December 2015 and March 2016. We chose DHBs of different sizes, in different regions, with different demographics.
1.12
We also collected data from the Ministry of Health (the Ministry) about people who had used mental health services in 2011/12, 2012/13, 2013/14, and 2014/15. The data did not include people's identities.
1.13
About 375,000 individuals received specialist mental health services during those four years. Of these, about 20,000 were aged 20-64 years and had at least one acute mental health admission to a hospital during the four years. We analysed data for this cohort of 20,000 people.
1.14
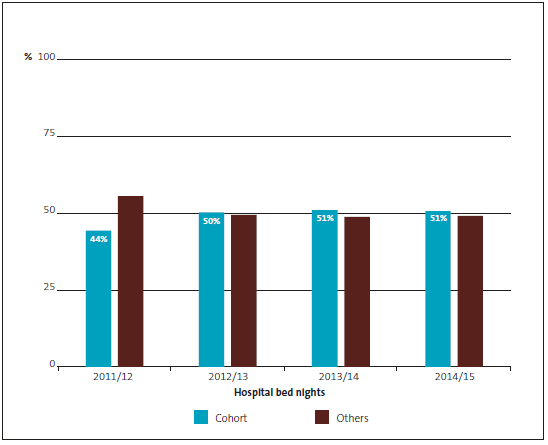
Although they made up a small proportion of all those receiving specialist mental health services, these 20,000 people accounted for almost half of all mental health bed nights1 (see Figure 2) and about 30% of all community contact activities2 (see Figure 3).
Figure 2
Percentage of bed nights for the cohort as a proportion of all mental health bed nights in all district health boards
Source: Our analysis of Ministry of Health data.
Figure 3
Percentage of community contact activities for the cohort as a proportion of all mental health community contact activities
Source: Our analysis of Ministry of Health data.
1.15
We analysed data about the contact the 20,000 people had with mental health services from 2011/12 to 2014/15.
1.16
We completed in-depth reviews of case files and clinical notes for 110 people treated in the three DHBs we visited and who were part of our national cohort of 20,000 people. Usually, we looked at the period from the person's admission to hospital to 90 days after leaving. If the person had a pattern of repeat admissions, then we looked at a wider time frame.
1.17
We interviewed more than 100 people in about 50 semi-structured interviews. These interviews included a mix of clinical and non-clinical staff, such as independent family, cultural, and patient advisers; staff from inpatient mental health teams; staff from community mental health teams; and staff in non-governmental organisations. Most of these people work for the three DHBs we visited. We also interviewed senior staff at the Ministry. We did not interview patients directly because we did not wish to potentially cause unnecessary distress.
1.18
We structured the interviews around our criteria, with a particular focus on matters raised by our case file reviews and early data findings.
1.19
We conducted a survey of just over 900 DHB staff, and achieved a response rate of just over 20%. We received responses from staff in 15 of the 20 DHBs.
1.20
We reviewed and analysed documentation and data, including financial information, from all 20 DHBs.
1.21
We held one workshop at Canterbury DHB, which was attended by about 16 clinical and non-clinical staff.
1.22
We reviewed some of the 500 stories that people submitted to the People's Mental Health Review.3 These stories gave us an insight into the views of people with a personal experience of mental health services in New Zealand. This helped us to understand and validate our findings.
1.23
We set up an external reference group to provide specialist advice to our audit team. Most of the group were clinicians (psychiatrists and registered mental health nurses) but we also included a patient representative and a Ministry data expert. The representatives on the group came from four different DHBs to the three that we visited.
1.24
We have also liaised with the relevant teams in the offices of the Ombudsman and of the Health and Disability Commissioner.
The structure of this report
1.25
In Part 2, we provide background information about the provision of acute mental health care, patterns of contact with mental health services, and mental health funding.
1.26
In Part 3, we consider how well planning was done before a person was discharged from an inpatient unit.
1.27
In Part 4, we discuss whether people received the support and follow-up they needed after they were discharged from an inpatient unit.
1.28
In Part 5, we examine the data and information that is currently available about acute mental health services. We explore opportunities for using that information to better understand how people with acute mental health problems are interacting with health services.
1: Total bed nights includes all types of mental health inpatient and residential care (such as acute, crisis, forensic, and residential) and also includes beds used by people aged 65 years or older.
2: Community contacts include any contact with community mental health services that is recorded in the data we received from the Ministry of Health.
3: These stories were analysed to identify key themes that are explored in the People's Mental Health Report, which was published by Action Station on 19 April 2017. See www.peoplesmentalhealthreport.com.