Part 5: Results of district health board audits for 2007/08
5.1
The 21 district health boards (DHBs) are fundamental to the delivery of health services in New Zealand. Nearly $9.032 billion of the just over $12.240 billion budgeted for government expenditure on health for 2008/09 is to fund health services from DHBs.
5.2
The Auditor-General is the auditor of the DHBs and their subsidiary organisations. In this Part, we briefly describe the DHBs and their operating environment, and the results of our annual audits of DHBs for the 2007/08 financial year.
What is the health sector?
5.3
The health sector contains 21 DHBs, set up in 2001 under the New Zealand Public Health and Disability Act 2000, which sets out the role and functions of DHBs. They are responsible for providing, or funding the provision of, health and disability services in their district, for the purpose, among others, of:
- improving, promoting, and protecting the health of communities;
- promoting the integration of health services, especially primary and secondary care services; and
- promoting effective care or support of those in need of personal health services or disability support.
5.4
Also included in the health sector are subsidiary companies that DHBs may have set up individually or jointly – for example, HIQ Limited, which provides information technology services to Capital and Coast and Taranaki DHBs. The DHBs share some of their planning, administrative, and quality assurance functions through shared service agencies and also through District Health Boards New Zealand.
5.5
DHBs have also been responsible, since the Primary Health Care Strategy was introduced in 2001, for setting up not-for-profit primary health organisations (PHOs). The DHBs have contracts with the PHOs for delivering and co-ordinating health care services for their enrolled populations. There are now about 80 PHOs around the country, with an enrolled population of about 3.9 million New Zealanders (95% of the population).
How are the district health boards funded and for what?
5.6
The overall level of funding appropriated for DHBs is determined by the Budget process, based on the Government’s spending priorities. For 2007/08, the funding was distributed to the health of older people (12.8%), mental health (12.1%), personal health care services (33.3%), and residential health and community-based health care services (41.8%).1
5.7
The amount of funding each DHB gets is determined by the size of its population, with additional socioeconomic and other risk factors taken into account. The funding covers the health and disability services that the DHB provides directly to its population, or indirectly through another provider (such as another DHB, or a private for-profit or not-for-profit provider such as a non-government organisation).
Size of the district health boards
5.8
DHBs vary considerably in the amount of funding they receive, and the size of areas and population they serve, as shown in Figures 6 and 7.
Figure 6
District health board areas
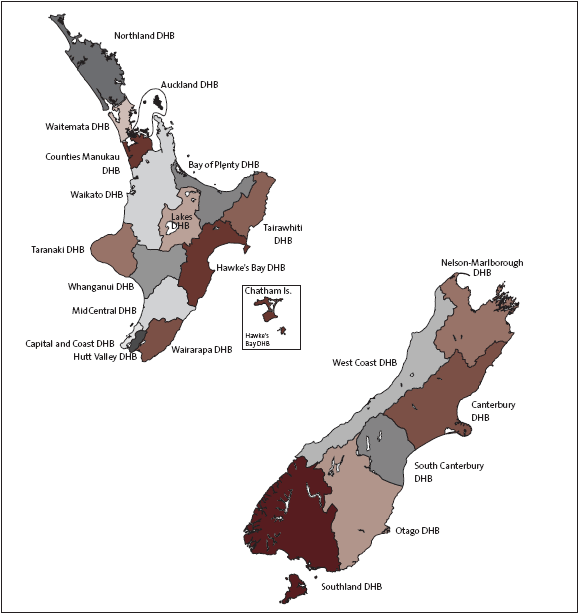
Source: Ministry of Health website, www.moh.govt.nz.
Figure 7
Population and funding of district health boards in 2007/08
| DHB | Populationa | Fundingb $m |
|---|---|---|
| North Island | ||
| Auckland | 442,720 | 839.9 |
| Bay of Plenty | 202,765 | 450.6 |
| Capital and Coast | 282,530 | 509.5 |
| Counties Manukau | 455,335 | 857.8 |
| Hawke’s Bay | 150,795 | 334.9 |
| Hutt Valley | 138,715 | 267.1 |
| Lakes | 103,015 | 219.3 |
| MidCentral | 164,685 | 350.9 |
| Northland | 150,593 | 357.5 |
| Tairawhiti | 44,663 | 107.1 |
| Taranaki | 105,103 | 240.6 |
| Waikato | 346,515 | 715.2 |
| Wairarapa | 39,295 | 93.8 |
| Waitemata | 513,840 | 948.8 |
| Whanganui | 62,158 | 159.8 |
| South Island | ||
| Canterbury | 483,945 | 960.1 |
| Nelson-Marlborough | 138,683 | 294.0 |
| Otago | 182,900 | 397.8 |
| South Canterbury | 53,600 | 128.0 |
| Southland | 110,645 | 223.1 |
| West Coast | 30,525 | 94.9 |
a: Population figures used to calculate 2007/08 population-based funding (Ministry of Health, 4 December 2008).
b: The Estimates of Appropriations 2007/08, B.5 Vol.1, pages 632-634.
Governance and accountability arrangements
5.9
Each DHB is responsible for identifying and providing for its district’s health needs, and is required to develop district strategic and annual plans that are consistent with New Zealand’s health and disability strategies.2 Each year, the DHB also publishes a Statement of Intent (SOI), a high-level, less detailed statement about how the DHB intends to address the health needs of its district. There is also increasing emphasis on inter-district planning and supply of health services.
5.10
Each DHB is governed by a board of seven elected members, and up to four members appointed by the Minister of Health (the Minister).3 DHBs are directly accountable to the Minister. As Crown Agents under the Crown Entities Act 2004, DHBs are required to give effect to government policy when directed by the Minister.4
5.11
The monitoring department is the Ministry of Health (the Ministry), which has a monitoring and support capability for DHBs within its Sector Accountability and Funding directorate. The Ministry maintains a monitoring regime with three different levels of intervention – standard monitoring, performance watch, and intensive monitoring.5 As at 30 June 2008, there were four DHBs on intensive monitoring (Capital and Coast, Hawke’s Bay, Southland, and Whanganui), and three on performance watch (Auckland, Waitemata, and West Coast). Since then, Auckland DHB has returned to standard monitoring, and Otago DHB has been placed on performance watch.
5.12
In addition to intensive Ministry monitoring, the Minister can make changes to how the DHB is governed, to help improve its performance.
5.13
This can be by appointing one or more Crown monitors to observe the decision-making processes of the board, to assist the board in understanding the policies and wishes of the Government, and to advise the Minister on any matters about the DHB, the board, or its performance.6 During 2007/08, Capital and Coast DHB and Whanganui DHB had Crown monitors in place.
5.14
If seriously dissatisfied, the Minister can dismiss the board and appoint a commissioner.7 During 2007/08, a commissioner was put in place in Hawke’s Bay DHB.
Annual audit of the health sector
5.15
The Auditor-General is the auditor of every public entity. Under section 15 of the Public Audit Act 2001, he audits the financial statements, accounts, and other information that each of the 21 DHBs, their subsidiaries, and District Health Boards New Zealand are required to have audited each year. He does not audit the PHOs, because they are not public entities. However, under section 16 of the Public Audit Act 2001, he can look at whether DHBs are fulfilling their responsibilities for primary health care.
5.16
The purpose of the annual audit is to give assurance that the public entity’s reports fairly reflect its financial and non-financial performance, and do not mislead the reader.
Financial performance of district health boards
5.17
Figure 8 sets out the financial performance of the 21 DHBs for the year ended 30
June 2008.
Figure 8
Summary of district health boards’ 2007/08 financial performance
| DHB | Revenuea $m | Expenditurea$m | Surplus (deficit)a $m | Deficit as % of revenue | Planned surplus (deficit)b$m | Variance to plan $m |
|---|---|---|---|---|---|---|
| Auckland | 1,530.3 | 1,527.9 | 2.4c | 0.1 | 2.3 | |
| Bay of Plenty | 505.3 | 507.7 | (2.4) | 0.5% | (2.3) | (0.2) |
| Canterbury | 1,181.0 | 1,197.8 | (16.9) | 1.4% | 0 | (16.8) |
| Capital and Coast | 719.9 | 760.2 | (40.7)c | 5.7% | (10.9) | (29.8) |
| Counties Manukau | 1,060.6 | 1,053.4 | 7.2 | (1.4) | 8.6 | |
| Hawke’s Bay | 383.9 | 390.6 | (6.7) | 1.8% | 0 | (6.7) |
| Hutt Valley | 363.8 | 373.3 | (9.4) | 2.6% | 0 | (9.4) |
| Lakes | 257.8 | 252.8 | 5.0 | (2.8) | 7.8 | |
| MidCentral | 452.1 | 456.2 | (4.1) | 0.1% | (4.4) | 0.3 |
| Nelson-Marlborough | 352.3 | 344.5 | 7.8 | (3.6) | 11.4 | |
| Northland | 409.8 | 409.0 | 0.7 | (0.0) | 0.7 | |
| Otago | 495.0 | 500.8 | (5.8)c | 1.2% | (3.3) | (2.5) |
| South Canterbury | 149.6 | 147.9 | 1.7 | 0 | 1.7 | |
| Southland | 246.3 | 249.2 | (2.9)c | 1.2% | (4.3) | 1.3 |
| Tairawhiti | 124.7 | 125.6 | (0.8)c | 2.3% | (0.4) | (0.4) |
| Taranaki | 271.6 | 272.9 | (1.3) | 0.5% | (1.9) | 0.6 |
| Waikato | 907.6 | 876.9 | 30.7 | 0.2 | 30.5 | |
| Wairarapa | 110.5 | 112.2 | (1.7) | 1.5% | 0.0 | (1.7) |
| Waitemata | 1,120.0 | 1,115.4 | 4.6 | (8.3) | 12.9 | |
| West Coast | 111.0 | 117.3 | (6.3) | 5.7% | (4.6) | (1.6) |
| Whanganui | 182.1 | 186.8 | (4.7) | 2.6% | (1.3) | (3.4) |
| Totals | 10,935.2 | 10,978.6 | (43.4) | (49.3) |
a: Audited results.
b: From the annual plans of DHBs. Figures provided by the Ministry of Health, December 2008.
c: In five cases (Auckland, Capital and Coast, Otago, Southland, and Tairawhiti DHBs), the surplus(deficit) is affected by including profits from associates that are additional to the revenue shown. For these five DHBs, the surplus(deficit) shown is therefore not the same as revenue less expenditure.
Overall financial stability
5.18
The board usually prepares the DHB’s financial statements on the basis of the “going concern” assumption (that is, on the basis that the DHB will continue to operate for the foreseeable future).
5.19
Sometimes, there are doubts about the appropriateness of the going concern assumption. Doubts can arise for many reasons, including:
- future funding not being agreed;
- potential for defaulting on loans or breaching borrowing covenants;
- significant liquidity or cash flow problems; or
- dependence on the continuing support of the Crown.
5.20
Where there are doubts, the board must be able to justify using the going concern assumption.
5.21
In some circumstances, to justify using the assumption, the board seeks assurances of financial support from the Crown (through the Minister). Such assurance is usually given in the form of a “letter of comfort”. In 2007/08, the Ministers of Health and Finance issued five letters of comfort. These were for:
- Capital and Coast DHB;
- Otago DHB;
- Southland DHB;
- West Coast DHB; and
- Whanganui DHB.
Audit opinions issued for the year ended 30 June 2008
5.22
Capital and Coast DHB received a non-standard audit report8 that contained an unqualified audit opinion but referred to future uncertainties about the outcome of negotiations for funding. Additional funding is needed to support this DHB's cash flow requirements for 2010 and beyond, because of significant forecast deficits.
5.23
The 2007/08 audit reports for all other DHBs contained unqualified audit opinions.
Environment, systems, and controls
5.24
The Auditor-General also comments on the management control environment, and financial and service performance systems and controls of DHBs, to highlight areas for improvement identified during the audit. Grades are assigned that directly represent the recommendations for improvement.9 Figures 9, 10, and 11 set out our grades for the management control environment, and financial information systems and controls for the DHBs, for the year ended 30 June 2008.10
5.25
Sixteen of the 21 DHBs were good or better in their management control environment. The rest needed improvement, and none were poor.
5.26
Two-thirds were good in their financial information systems and controls. Again, the rest needed improvement, and none were poor.
5.27
These results are very similar to the 2006/07 grades.11
Figure 9
Summary of grades for each district health board’s management control environment
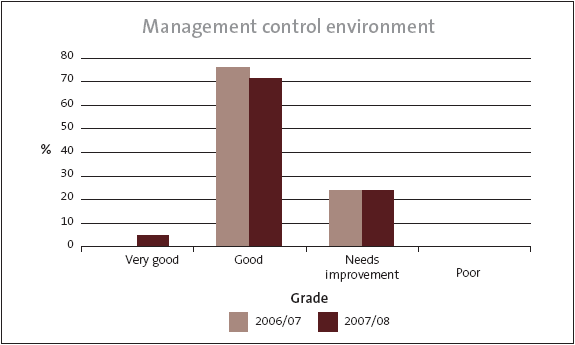
Figure 10
Summary of grades for each district health board’s financial information systems and controls
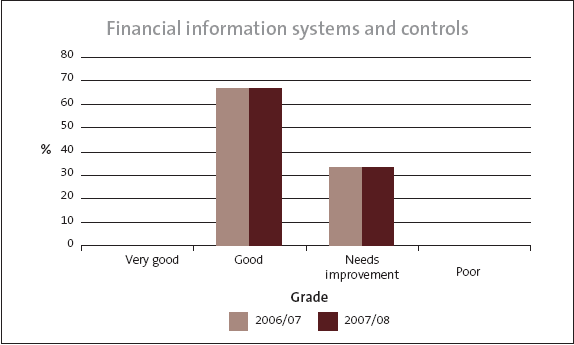
Figure 11
Grades for each district health board
| DHB | Management control environment | Financial information systems and controls |
|---|---|---|
| Auckland | Very good | Good |
| Bay of Plenty | Good | Needs improvement |
| Canterbury | Good | Good |
| Capital and Coast | Needs improvement | Needs improvement |
| Counties Manukau | Good | Good |
| Hawke’s Bay | Needs improvement | Needs improvement |
| Hutt Valley | Needs improvement | Good |
| Lakes | Good | Good |
| MidCentral | Good | Needs improvement |
| Nelson-Marlborough | Good | Good |
| Northland | Good | Good |
| Otago | Good | Good |
| South Canterbury | Good | Good |
| Southland | Good | Good |
| Tairawhiti | Good | Needs improvement |
| Taranaki | Good | Good |
| Waikato | Needs improvement | Needs improvement |
| Wairarapa | Needs improvement | Good |
| Waitemata | Good | Good |
| West Coast | Good | Good |
| Whanganui | Good | Needs improvement |
Key areas of audit focus in the 2007/08 annual audits
5.28
Two key areas of focus for the audits of DHBs in 2007/08 were:
- information about future operating intentions; and
- procurement policies and practice.
Results of review of information about future operating intentions of district health boards
5.29
We want to see continuous improvement in DHBs’ SOIs. Each year, we review DHBs’ SOIs during the audit. In 2007/08, this was supplemented by a desk-based review of the final 2008/09 SOI. Our aim is for DHBs to have a more consistent and comprehensive approach to performance reporting. A DHB should be using the same performance information as the basis for its statement of service performance (SSP) that managers use to make decisions. DHBs also need to use adequate processes to set the measures – for example, benchmarking or trend analysis – and to consult.
5.30
The focus of our work is on:
- ensuring that the SOI complies with relevant legislative requirements;
- ensuring that the forecast output information in the forecast SSP is consistent with any forecast output information included in the Estimates of Appropriation;
- assessing the “appropriateness” of the performance measures (taking into account comments provided to DHBs on the 2007/08 SOI); and
- considering whether there are any other issues with the measures and targets that may affect the audit opinion on the SSP – in particular, whether the measures can be audited.
5.31
Our review identified that the documents produced could be improved (in some cases significantly) by:
- clearly explaining the links between the services that DHBs are responsible for and the impacts and outcomes that they are seeking to achieve (that is, the “performance story”);
- ensuring that the outcomes described in the SOI are consistent with the statutory definition of an outcome, and are clearly identified;
- ensuring that the outputs described in the SOI relating to the goods and services that the DHB is responsible for providing to third parties are appropriately aggregated into meaningful output classes and cover all the significant services funded (information about internal processes, milestones, and organisational improvements is useful to the reader, but should not be included as outputs in the forecast SSP); and
- including performance measures for both outputs and outcomes. These should cover a number of the dimensions of performance, including quality, quantity, and timeliness, together with targets, baseline data, and other comparative information that will help the reader put the DHB’s performance in context.
5.32
We continue to work with the monitoring department (the Ministry) and the central agencies (the Treasury and State Services Commission) to provide advice and support to a working group set up by the DHBs in response to our feedback. The working group intends, in particular, to address the definition of outputs and of output classes in the DHB sector. It is also giving attention to the general structure of the SOIs, with the aim of clarifying the performance story. We expect this work to result in improvements to the 2009/10 and 2010/11 SOIs, when we will, for the first time, be grading service performance information and associated systems and controls.
5.33
We are aware that the health sector has some particular issues with the number of accountability documents that it is required to produce. The Ministry has been reviewing the sector accountability documents. We intend to discuss with the Ministry and the DHBs how to achieve more clarity in sector accountability documents.
Audit findings on managing procurement
5.34
Procurement covers all the business processes associated with purchasing, from policies through to procurement practice. We have a particular interest in the effective and efficient procurement of goods and services when this involves the use of public resources, and have published good practice guidance on procurement.12
5.35
In last year’s report,13 we had a number of criticisms of the procurement policies that we examined in the 2006/07 audit. In 2006/07, we looked at a sample group of DHBs’ procurement policies and found they needed improvement. We therefore reviewed procurement policies and practices in DHBs during the 2007/08 annual audit (see Part 9).
5.36
We considered procurement in its widest sense from business case to contract end, consistent with our guidance. We considered purchasing arrangements (contracts) with providers and suppliers of goods and services for both conventional and relational purchasing,14 including when purchasing services from non-government organisations. We did not cover grant arrangements, even if those arrangements were documented in a contractual form.
5.37
Procurement expenditure varies widely throughout the DHBs. Some are large entities with total annual expenditure of more than $1 billion. Others are much smaller, spending only $100 million annually. However, it is clear that procurement represents the greatest proportion of annual expenditure for all DHBs. This is so whether that proportion is 70%, as it is for one DHB, or only 49%, as it is for those at the lower end of the range. It is therefore crucial to DHBs’ effective operation that procurement is well managed.
5.38
Because of this, and the level of concern about procurement in the health sector in particular, we carried out a more detailed review of procurement policies and practice in DHBs in 2007/08 and analysed the areas where improvements were required.
Areas for improving procurement policies
5.39
We examined nine areas to identify where improvements could be made in procurement policies:
- whether the policies cover all the DHB’s procurement activities, who approved the policies, and whether they are available to the relevant staff (that is, status and availability);
- general provisions (for example, whether they reflect the essential principles set out in our guidance);
- planning and methods (for example, whether they include an appropriate range of procurement approaches);
- legal considerations (for example, whether they reflect public law obligations and caution about process-related contract obligations);
- ethical provisions (for example, whether they deal with conflicts of interest);
- economic considerations (for example, requirements to ensure value for money);
- whether they take sustainability into account;
- risk management (for example, whether they include provisions for identifying, recording, assessing, and managing risks); and
- processes and management (for example, whether open tendering is required for conventional procurement).
5.40
All of the DHBs were deficient in at least one of these areas (see Figure 12).
5.41
We assessed which of the nine key areas DHBs were deficient in. Figure 13 sets out our results for the 21 DHBs.
Figure 12
Number of district health boards with procurement policy deficiencies
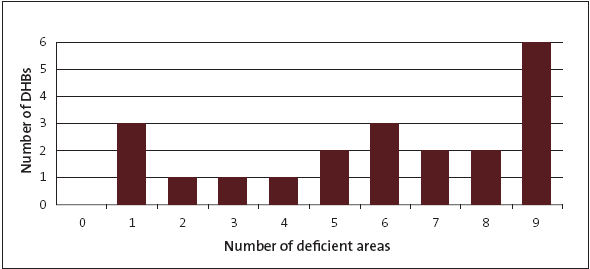
Figure 13
Number of district health boards with procurement policy deficiencies, by type
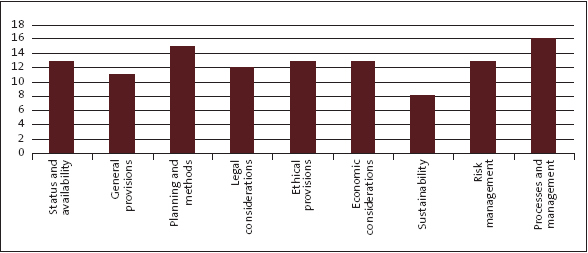
5.42
Most of the deficiencies in procurement policies were in processes and management, planning and methods, and ethical provisions. In particular, better guidance is needed in the policies about:
- when to tender;
- dealing with late tenders;
- risk management processes;
- managing fraud and corruption risks;
- dealing with gifts and hospitality when they are associated with procurement;
- managing the risk of potentially unfair advantage when former employees seek to be contractors;
- management of intellectual property considerations; and
- obtaining value for money.
Areas for improving procurement practice
5.43
We assessed procurement practice for the first time in 2007/08. We asked DHBs to complete a self-assessment of their procurement practice based on expenditure with external suppliers and providers, covering six areas:
- management arrangements (for example, structure of procurement management, staff capacity for procurement, management of contract information);
- procurement strategy (for example, strategic planning, selecting a procurement approach to suit the particular circumstances);
- ethical and legal considerations (for example, managing conflicts of interest);
- procurement processes (for example, whether open tendering is used where practical and appropriate, how value for money is achieved);
- ongoing management of contracts (for example, approach to monitoring contracts); and
- continuous improvement (for example, recent improvements, having established some priorities for future improvement).
5.44
Figure 14 shows the number of DHBs by the number of areas of deficient procurement practice.
Figure 14
Number of district health boards with deficiencies in procurement practice
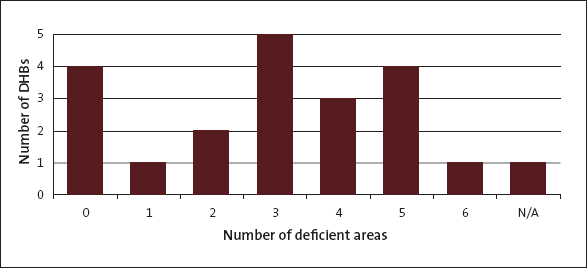
5.45
We assessed which of the six areas of procurement practice the 21 DHBs were deficient in. Figure 15 sets out our results.
Figure 15
Number of district health boards with deficiencies in procurement practice, by type
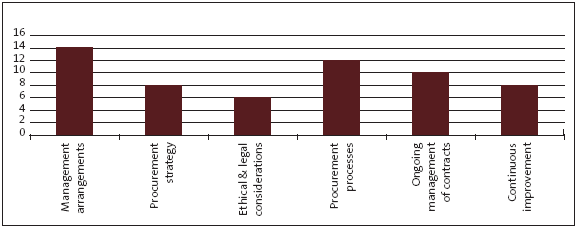
5.46
One particular problem was a lack of consistency between procurement operations in each of the DHB’s main areas of activity – planning and funding (buying services from other providers), and providing services. There was also a lack of sharing of available expertise and knowledge across these procurement areas. This means the DHBs are not making the most of staff capacity and a corporate approach. In one DHB in particular, this affected its ability to provide us with information on its procurement operations for all of its activities.
5.47
The self-assessments that DHBs completed, our benchmarking, and our subsequent audit work highlighted the following issues in the six areas of procurement practice:
- Management arrangements: Procurement does not have the emphasis in DHBs that its value warrants, and there are limited numbers of procurement professionals in DHBs throughout the country. Procurement in DHBs is fragmented between the separate business units and “arms” (all DHBs separate their management of corporate procurement, procurement for providing services, and procurement for funding other providers of services). This is not necessarily an issue if the information systems are appropriate, policies and guidance are clear, and staff are trained and share information. It is not always clear that this is the case. We expected a stronger focus on professional development of existing staff. Apart from the deficiencies already noted, most DHBs have up-to-date procurement policies. How they ensure compliance with their policies is less clear. Most DHBs have a contract management system, but, despite this, access to good quality management information is limited.
- Procurement strategy: Most DHBs are members of joint procurement arrangements, and these offer good potential for leveraging buying power and achieving value for money. However, there is still scope to benchmark the costs actually incurred to indicate areas where some DHBs may be using services more effectively and efficiently. Also, information on the cost of health services the DHB provides is typically more complete than information about the services that it funds others to do. Arrangements for consulting service users to inform procurement decisions – for example, on what products and services to buy – tend to be under-developed.
- Ethical and legal considerations: While DHBs increasingly take a proactive approach to managing conflicts of interest, this remains an area that will require vigilance. Most DHBs have a process for managing tenders appropriately, covering aspects such as managing communications, ensuring confidentiality, security, and opening of tenders. Application of the process is somewhat varied.
- Procurement processes: All DHBs report that their policy requires a competitive process for purchases above certain thresholds or in certain circumstances. However, there does not appear to be a robust focus on value for money when DHBs do not use a contestable process for procurement. They report that they usually manage and demonstrate value for money through price checking against other DHBs, monitoring service delivery, and quality audits. It is unclear how systematic these processes are. Most DHBs report that they have some contracts with no specified completion date, and no provision to terminate the contract if need be. “Evergreen” contracts are not usually good practice. DHBs should have a structured programme of reviewing such contracts. DHBs should either put contracts on a more conventional basis where appropriate, or make sure that there are mechanisms in place to achieve value for money within the contract’s framework, and identify and manage any inherent risks. Most DHBs have guidance available on what procurement-related records should be kept. However, the retention is often fragmented, with a mixture of hard copy and electronic records that are incomplete.
- Ongoing management of contracts: DHBs have contract management arrangements, but there are significantly varying practices in what is done to monitor and manage contractor performance. They could increase the scope, frequency, and consistency with which this is done, and the level of reporting that goes to senior managers and the board. Contract management also needs to be based on risk.
- Continuous improvement: All DHBs report recent and ongoing improvements to their procurement systems and processes. Most DHBs have put their efforts into improving procurement systems and processes, recruiting the right staff for key procurement roles, and developing competencies in all their procurement staff. Our work indicates that progress in these three areas needs to continue.
5.48
We were pleased to note some improvements in procurement policies and practice in the DHB sector, though there is still a need for further improvement. We have informed the board and management of the individual DHBs of our findings for 2007/08, and will be focusing our audit for 2008/09 on whether DHBs have addressed the areas for improvement.
5.49
We are also in the process of carrying out an in-depth performance audit of three DHBs’ procurement policies and practice. The performance audit is intended, along with results of our other audit work on procurement, to provide Parliament with an understanding of how effectively these DHBs are managing procurement, and to add value to the sector.
1: The Estimates of Appropriations 2007/08, B.5 Vol.1, page 640.
2: See section 38, New Zealand Public Health and Disability Act 2000.
3: Section 28(1)(a), Crown Entities Act 2004.
4: Section 7(1)(a), Crown Entities Act 2004.
5: Briefly stated, standard monitoring is used when a DHB is in a sound financial position, has supported accountability arrangements in place, and is complying with requirements in a timely manner. DHBs are under a performance watch when there is some non-compliance or deterioration in performance. Intensive monitoring occurs when a DHB continues to be non-compliant or deteriorates in the performance watch requirements, or a single event creates a material risk. There are two further intervention stages – intermediate governance action, and direct governance action if the Minister is seriously dissatisfied with the Board’s performance.
6: Section 30, New Zealand Public Health and Disability Act 2000.
7: Section 31, New Zealand Public Health and Disability Act 2000.
8: See Part 4.
9: See Part 2 for more information about the assessment scale.
10: We did not grade service performance information and associated systems and controls for 2007/08.
11: Central government: Results of the 2006/07 audits, page 31.
12: Procurement guidance for public entities, June 2008.
13: Central government: Results of the 2006/07 audits, May 2008, Part 4.
14: Procurement guidance for public entities, June 2008, Part 6.
page top